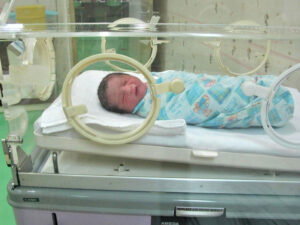
For some pregnant women, medical factors mean a maternal fetal medicine (MFM) specialist becomes involved. An MFM specialist is an OBGYN with extra training to manage a high-risk pregnancy.
A high-risk pregnancy is one where certain medical, fetal, or pregnancy-related factors increase the chance of complications for you or your baby. Many high-risk pregnancies are identified early. Others develop as pregnancy progresses. High-risk pregnancies are referred to a MFM specialist to monitor closely, to help reduce complications.
Risk is a spectrum rather than a single diagnosis.
Some women’s pregnancies are already high risk because of existing health conditions. Others move from a low-risk to a high-risk category as new issues appear. Changes in symptoms, test results, or how your baby develops can shift how doctors classify your maternal fetal medicine care needs.
Early monitoring is essential for high-risk pregnancies. Regular check-ins allow doctors to track emerging complications, adjust care plans, and reduce unnecessary stress for pregnant women. Your care team can then help you have a healthy pregnancy – protecting both your health and your baby’s health.
Let’s look into high-risk pregnancy care.
Table of contents
What Makes Pregnancy High Risk
Understanding Your Health Risk Factors During Pregnancy
Fetal Conditions That Require Specialized Monitoring
What is a Maternal Fetal Medicine Specialist?
When Are Women Referred to a Maternal Fetal Medicine Specialist
Advanced Testing and Diagnostic Imaging Explained
More About Genetic Conditions and Pregnancy Risk
The Importance of Access to a Neonatal Intensive Care Unit (NICU)
High-Risk Pregnancy Care and Emotional Support
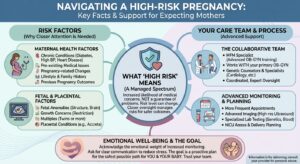
What Makes a Pregnancy High Risk
A pregnancy may be considered high risk when certain maternal or fetal factors increase the likelihood of medical concerns. These factors don’t guarantee problems, but they do raise pregnancy risks that benefit from closer medical oversight. Many high-risk pregnancy situations are common and manageable when identified early and followed carefully.
From a maternal perspective, chronic conditions such as high blood pressure, diabetes, heart disease, blood clotting disorders, and autoimmune disorders can significantly affect pregnancy.
In some cases, changes related to being pregnant, rather than the condition itself, raise concern and require closer observation.
Fetal factors also play an important role in determining whether a pregnancy is high risk. These include fetal anomalies, concerns about baby’s growth, or carrying twins or higher order multiples.
Each situation presents different pregnancy risks, and MFM specialists adjust care plans based on how your baby develops over time.
Importantly, high risk doesn’t describe a single moment or diagnosis. Risk can increase or decrease throughout pregnancy. And many women move along this spectrum as new information becomes available.
Understanding what places a pregnancy into a high-risk category helps doctors anticipate complications and tailor care to protect both you and your baby.
Understanding Your Health Risk Factors During Pregnancy
Health risk factors help explain why some pregnancies need closer attention than others. Many health conditions are manageable on their own. But they can become more complex when combined with the physical demands of pregnancy.
Chronic issues such as diabetes, autoimmune disorders, or other ongoing medical condition concerns may increase risk if they’re not carefully managed throughout pregnancy.
In addition, family history of certain conditions or previous pregnancy outcomes can influence how doctors assess current risk pregnancy and future pregnancies.
Lifestyle factors, including nutrition, activity level, and access to ongoing medical support, may also affect pregnancy in ways that are not always obvious early on.
These overlapping factors for pregnant women help explain why care plans need to be individualized and proactive to reduce complications.
They allow doctors to adjust your treatment and care for high-risk needs, and respond quickly. Effective care from a maternal fetal medicine specialist protects your health, your baby, and your overall well-being as pregnancy progresses.
But don’t assume you’ll have problems! Providers have a clear roadmap for managing risk and reducing uncertainty throughout your pregnancy.
Fetal Conditions That Require Specialized Monitoring
Some pregnancies require closer observation because of how your baby is developing. These conditions increase risk and need more frequent evaluation. Doctors can then respond early before complications arise.
For example, specialized ultrasound may show fetal anomalies involving your baby’s heart, brain, or other organs.
Your OBGYN or maternal fetal medicine specialist may have concerns about your baby’s growth, such as growth restriction or patterns that suggest your baby may not be receiving enough oxygen or nutrients.
Tracking these changes over time helps an MFM specialist determine how to adjust your pregnancy care.
Placental conditions are another important factor.
Issues such as placenta accreta (abnormal attachment of the placenta) can significantly increase risk, particularly later in pregnancy and during birth. Placenta accreta requires close monitoring and careful planning. In some high-risk situations, identifying placenta accreta early allows doctors to coordinate specialized care and reduce the chance of serious complications.
By combining detailed imaging with regular follow-up, care teams can better understand how fetal conditions may affect the course of pregnancy, keeping both you and your baby as safe as possible.
What is a Maternal Fetal Medicine Specialist?
A maternal fetal medicine specialist is an obstetrician with advanced training in managing complex high-risk pregnancies, including conditions that affect both mother and baby. The MFM has completed 4 years of OBGYN residency, followed by a 3-year MFM Fellowship program.
Their focus is on anticipating challenges, reducing risk, and supporting your safest possible path through pregnancy and birth.
Doctors trained in maternal fetal medicine work closely with your primary OBGYN and other specialists to provide coordinated, expert oversight.
In many cases, care involves these multiple doctors because they contribute different expertise, from cardiology to endocrinology, depending on the underlying medical condition. This collaborative care team approach ensures you get informed, timely decisions centered on both your health and your baby’s needs.
When Are Women Referred to a Maternal Fetal Medicine Specialist?
A maternal fetal medicine specialist referral happens when concerns such as high blood pressure, diabetes, placental disorders, or prior pregnancy complications raise concerns.
Referral doesn’t replace your OBGYN. Maternal fetal medicine adds another layer of insight and advanced care, especially for evolving risk pregnancy scenarios.
Guidelines from organizations such as the American College of Obstetricians and Gynecologists support this team-based model, which is also reflected in academic centers like Weill Cornell Medicine.
Bringing together experienced doctors, highly trained specialists, and a coordinated team helps maternal fetal medicine deliver expert care for women who need care for high-risk situations throughout pregnancy.
Advanced Testing and Diagnostic Imaging Explained
Advanced testing helps doctors understand how your pregnancy is progressing and whether emerging concerns need intervention. In high-risk situations, routine screening may not provide enough detail. Which is why advanced testing and advanced imaging play an important role in guiding care decisions.
High-resolution ultrasound allows doctors to evaluate structure, movement, and circulation in greater detail. When an ultrasound shows changes in anatomy or development, providers can assess how those findings may affect your baby’s growth and overall health.
They may use additional imaging to monitor blood flow, placental function, or how well your baby is tolerating the pregnancy.
Laboratory evaluation also supports clinical decision-making.
A blood test may be used to assess infection risk, clotting concerns, or how your body is responding to conditions such as diabetes – or acquiring gestational diabetes. Monitoring blood sugar trends helps doctors treat complications and reduce risk to you and your baby.
Together, imaging and testing allow doctors to identify pregnancy concerns early and refine your care plans.
More About Genetic Conditions and Pregnancy Risk
Some pregnancies involve an increased level of risk because of inherited or chromosomal factors.
Genetic conditions may be known before conception or identified during pregnancy through screening and diagnostic evaluation.
In other cases, a genetic disorder is suspected later in pregnancy based on imaging findings, lab results, or a known family history.
These situations can feel overwhelming. But clear information helps guide next steps.
When genetic concerns are identified, genetic counselors play an important role in helping patients understand what the findings mean. Genetic counseling explains:
- How specific genetic conditions may affect pregnancy
- The likelihood of recurrence in future pregnancies
- What monitoring or planning may be helpful
This supports informed decision-making without assuming a single outcome for your baby.
Advances in screening and diagnostic tools also support proactive care. In some cases, testing is part of preconception counseling. In others, it becomes relevant later in pregnancy as new information emerges.
Understanding genetic risk factors allows doctors to tailor monitoring, coordinate appropriate treatment, and plan your delivery or specialist newborn care.
With the right support, most women navigate genetic concerns while maintaining focus on their baby, their health, and the safest possible course through pregnancy.
The Importance of Access to a Neonatal Intensive Care Unit (NICU)
For some high risk pregnancies, certain medical or fetal concerns increase the chance that your baby may need immediate support after birth – which is why access to a neonatal intensive care unit can be a critical part of planning. It reduces uncertainty and allows doctors to prepare proactively.
The Neonatal Intensive Care Unit
A neonatal intensive care unit provides specialized newborn care for babies born pre-term (“early”), or who have medical complications.
Stella Mattina MFM specialists work at hospitals with a dedicated NICU – including Medical City Dallas, Methodist Dallas Medical Center, and Medical City Arlington.
Some concerns identified during pregnancy suggest your baby may need monitoring right away to ensure they’re getting enough oxygen and adjusting safely after birth.
Planning for these possibilities allows care teams to quickly provide additional support.
Delivery planning is also about coordination. When a pregnancy involves higher risk, doctors work together to determine the safest timing and setting for labor and birth.
This coordinated approach supports a smooth path from prenatal care to newborn care – assuring your baby receives the highest level of attention if complications arise.
Having a clear prenatal and neonatal plan also brings peace of mind. You can focus less on uncertainty and more on welcoming your baby in an environment that’s safe and stable from the first moments. This is the best possible outcome!
High-Risk Pregnancy Care and Emotional Support
High-risk pregnancy care with maternal fetal medicine supports you medically but can carry emotional weight from increased monitoring.
In a high-risk pregnancy, expect more frequent appointments and additional testing, imaging, or maternal fetal medicine specialist input, perhaps including treatment.
You should also expect clear communication to reduce the impact of this schedule. At appointments, you can ask your care team to explain findings, outline next steps, and help you understand how decisions support your baby and your own health.
For many patients, this reduces stress and builds trust throughout pregnancy.
Emotional support is also part of comprehensive care. Managing medical risk while navigating fear or stress can affect your mental health. Compassionate care recognizes the link between emotional and physical well-being. With this in place, you can engage in care plans with specialists who protect you and your baby through pregnancy, labor, and birth at the highest level.
Stella Mattina Has Experts For High-Risk Pregnancy Care in Dallas
If you’re pregnant and looking for a high risk pregnancy doctor or a good OBGYN in Dallas who provides coordinated, compassionate care, we have experienced doctors and maternal fetal medicine specialists fully focused on safe outcomes for complex pregnancies.
And if you’re searching for an experienced OBGYN in Dallas or a trusted Gynecologist Dallas who other women rely on, book an appointment today.

Dr. Joshua Weiss
Dr. Joshua Weiss attended The University of Texas in Austin and The University of Texas Southwestern Medical School in Dallas. Upon completion of his OBGYN residency at Methodist Hospital of Dallas, he moved to New York City where he performed his maternal-fetal medicine fellowship at Columbia University. He is board certified in both obstetrics & gynecology and maternal-fetal medicine. He began the practice of maternal-fetal medicine in Dallas in 2003. In 2006, he opened his current office, Joshua L. Weiss, M.D. Associated.